Photobiomodulation (PBM), also known as low-level laser therapy (LLLT), is a medical technique that uses low-energy light to influence and improve biological processes in cells and tissues.
The goal of photobiomodulation is to stimulate cell activity, reduce inflammation, promote tissue repair, and relieve pain, without causing damage or heating the tissues.
This accelerates the natural healing process.
Light absorption by cells:
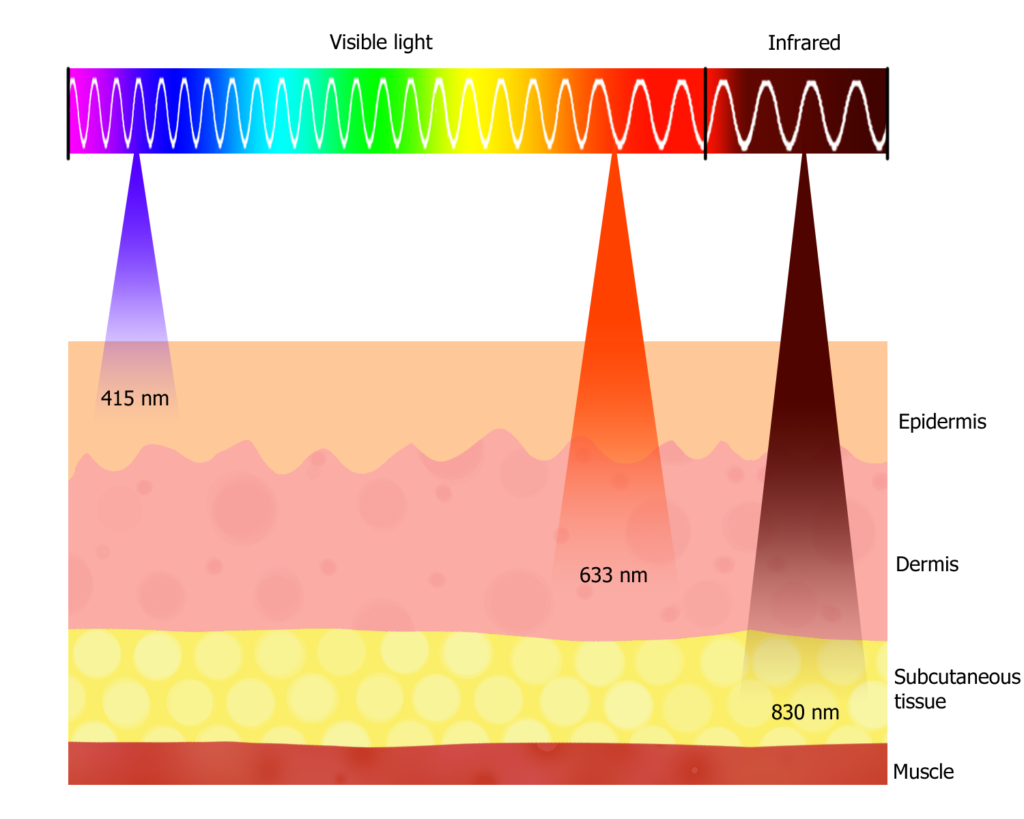
In PBM, specific wavelengths of light—typically red (600–700 nm) and near-infrared light (700–1200 nm)—are directed at the treatment areas.
In the case of the B-Cure laser, this involves infrared light with a wavelength of 808 nm. This light is generated by a solid-state laser diode.
This diode produces a coherent beam of light capable of penetrating the skin.
The light energy is absorbed by the mitochondria of the cells, thereby increasing energy production (in the form of ATP) within the cells.
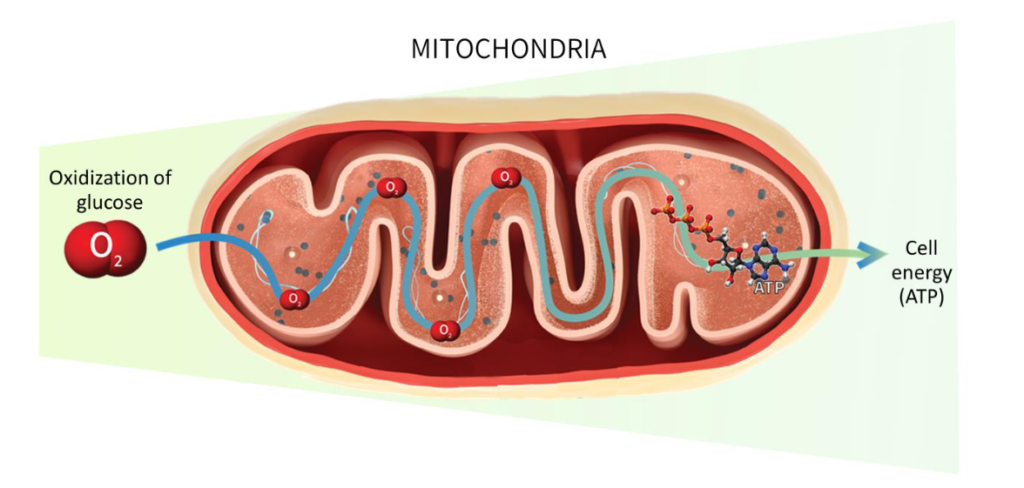
Biological responses:
This increased production of ATP (adenosine triphosphate) stimulates various cellular processes, such as protein synthesis, cell proliferation (the multiplication of cells), and the reduction of oxidative stress.
This helps promote healing and reduce inflammation and pain.
For a scientific explanation, see PubMed.
Applications of photobiomodulation (PBM)
– Pain relief: PBM is often used to relieve pain by inhibiting inflammatory processes and stimulating endorphin production.
– Anti-inflammatory effects: PBM can reduce inflammation levels, which is beneficial for conditions such as arthritis and sports injuries.
– Wound healing: PBM can accelerate wound healing by improving cell regeneration and tissue repair.
In essence, photobiomodulation is a safe and non-invasive therapy that uses light to help the body heal and recover.
Below are thermal images of hands, taken immediately after and 10 minutes after completing a 5-minute application with the B-Cure laser on the radial artery (outer side of the wrist).
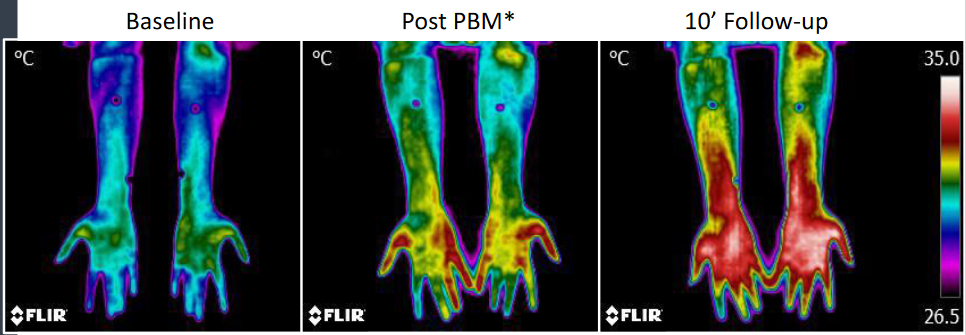
Note that the increase in skin temperature continued to rise even after the PBM was discontinued, suggesting the potential to improve tissue perfusion*.
According to the literature, however, an increase in skin temperature resulting from heating (e.g., with a hot water bottle) lasts no longer than a few minutes after the heat source is removed.
The history of photobiomodulation
The Hungarian physician and surgeon Endre Mester (1903–1984) is credited with discovering the biological effects of low-power lasers, a few years after the invention of the ruby laser in 1960 and the invention of the helium-neon (HeNe) laser in 1961.
Mester accidentally discovered that low-power ruby laser light could regrow hair while attempting to repeat an experiment that demonstrated that such lasers could reduce tumors in mice.
The laser he used was defective and not as powerful as he thought. It had no effect on the tumors, but he noticed that in the areas where he had shaved the mice to conduct the experiments, the hair on the treated mice grew back faster than on the mice in the control group.
He then demonstrated that low-level HeNe light could accelerate wound healing in mice.
By the 1970s, he was applying low-level laser light to treat people with skin ulcers.
In 1974, he founded the Laser Research Center at Semmelweis Medical University in Budapest.
Mester originally called this approach “laser biostimulation,” but it soon became known as “low-level laser therapy,” and with the adoption of light-emitting diodes by those studying this approach, it became known as “low-level light therapy,” and to resolve the confusion surrounding the exact meaning of “low-level,” the term “photobiomodulation” emerged.
Starting in 1992,
his research became more accessible to the broader scientific community, and since then, PBM Therapy has been studied in much greater detail. There are now hundreds of randomized controlled trials (RCTs), thousands of articles published in respected peer-reviewed journals, and hundreds of research reviews.
Much of this has been published on PubMed Central® .
In addition, studies have also been conducted using the B-Cure laser; you can find them here.
Footnotes and sources: